Varicose veins, typically found in the lower legs, are enlarged veins that affect 20-30% of adults, with a higher prevalence among older individuals. While often a cosmetic concern, they can also cause discomfort and complications such as leg swelling, bleeding, blood clots, severe skin changes, and chronic wounds if untreated. Discover effective varicose veins treatment available for patients.
At Certified Foot and Ankle Specialists, we prioritize efficient treatment for this condition, especially for our active South Florida patients who frequently wear shorts year-round. If you’ve noticed varicose veins in your lower extremities, don’t delay scheduling an appointment with the best podiatrists near you. Our vein specialists can effectively treat the condition, resulting in the reduction or complete elimination of unsightly veins, helping you get back to all the outdoor activities you love.
What are Varicose Veins?
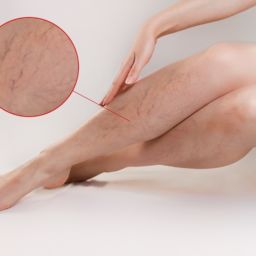
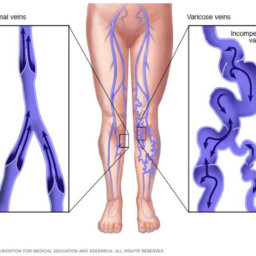
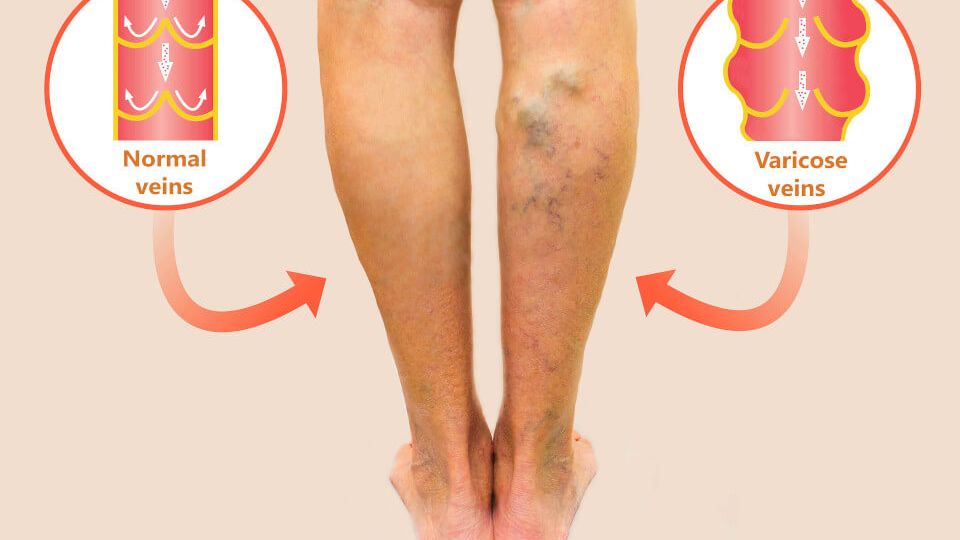
Varicose veins are enlarged, twisted, and bulging veins that appear just beneath the skin’s surface, most commonly in the legs and feet. These rope-like, bluish-purple veins occur when blood pools in the veins due to weakened or damaged vein walls and faulty valves that normally prevent blood from flowing backward.
Unlike healthy veins that efficiently transport blood back to the heart, varicose veins develop when the one-way valves inside the veins fail to function properly. This valve dysfunction causes blood to flow backward (reflux) and accumulate in the vein, leading to increased pressure and the characteristic enlarged, twisted appearance.
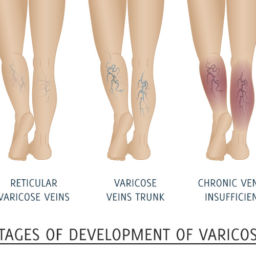
Varicose veins are different from spider veins, which are smaller, thinner, and closer to the skin surface. While spider veins are primarily a cosmetic concern, varicose veins can cause significant discomfort and lead to serious health complications if left untreated. The condition affects millions of Americans, with women being more susceptible than men due to hormonal factors and pregnancy-related changes.
These problematic veins typically develop in the superficial venous system of the legs, particularly in areas where veins are subject to higher pressure when standing or walking. The great saphenous vein, which runs from the ankle to the groin, and the small saphenous vein, located on the back of the calf, are commonly affected areas where varicose veins originate.
Symptoms and Causes of Varicose Veins
Common Symptoms of Varicose Veins
Varicose veins can present with both visible and physical symptoms that range from mild cosmetic concerns to debilitating discomfort.
- Visible symptoms include bulging, twisted veins that appear dark blue or purple beneath the skin, particularly prominent when standing. You may also notice skin discoloration around the affected veins, ranging from brown patches to reddish areas, especially around the ankles.
- Physical symptoms often worsen throughout the day and may include aching, throbbing, or cramping pain in the legs, particularly after prolonged standing or sitting. Many patients experience a heavy, tired feeling in their legs, along with burning or itching sensations around the affected veins. Swelling in the lower legs and ankles, especially at the end of the day, is another common complaint.
- Advanced symptoms that require immediate medical attention include skin ulcers or sores near the ankles, bleeding from varicose veins, and hard, tender lumps beneath the skin indicating possible blood clots. Some patients also experience restless leg syndrome, making it difficult to sleep comfortably.
Primary Causes and Risk Factors
- Age and Gender: As we age, vein walls and valves naturally weaken, making varicose veins more likely to develop. Women are disproportionately affected due to hormonal changes during pregnancy, menstruation, and menopause, which can relax vein walls and increase the risk of valve dysfunction.
- Genetic Predisposition: Family history plays a significant role, with individuals having close relatives with varicose veins being at higher risk. This genetic component affects the strength and structure of vein walls and valves from birth.
- Lifestyle and Occupational Factors: Prolonged standing or sitting, especially in occupations like teaching, nursing, or office work, increases venous pressure and contributes to valve failure. Lack of regular physical activity can also weaken the muscle pumps that help push blood back to the heart.
- Physical Factors: Obesity increases abdominal pressure, which can impede blood flow from the legs back to the heart. Pregnancy not only increases blood volume but also adds pressure on the pelvic veins, while hormonal changes relax vein walls.
- Medical Conditions: Previous blood clots, deep vein thrombosis, or other vascular conditions can damage veins and increase the likelihood of developing varicose veins. Chronic constipation can also increase abdominal pressure and contribute to the condition.
Understanding these symptoms and causes helps patients recognize when to seek professional evaluation and treatment, preventing the progression to more serious complications.
Why do Varicose Veins Occur?
Before we get into treatment options, it is important to understand why varicose veins develop in the first place. The veins in your legs’ main function is to bring blood in a one-way direction from the feet to the heart. This is conditioned upon a very well-coordinated action of muscle contractions and vein valve function. During ambulation, muscle contractions propel the blood to flow against gravity; meanwhile, tissue valves inside your veins open and close in a sequential manner to avoid the blood from flowing in the opposite direction. At rest, these valves remain closed. Any condition disrupting this coordinated effort of muscle contraction and valve closure can trigger backward blood flow or reflux. Reflux within the superficial veins is the main reason why people develop varicose veins. Family history, advanced age, female sex, obesity, and occupation are the most common conditions associated with venous reflux and varicose veins. Vein walls and valves of patients with the above conditions weaken over time causing vein enlargement and reflux. Varicose veins are enlarged, twisted, and raised veins below the skin surface.
Treating Your Varicose Veins Conservatively
After diagnosing your varicose veins, your vein specialist or podiatrist will recommend conservative options first. This includes compression wraps or stockings, and tips to improve your circulation overall, like exercise, leg elevation, and avoiding long periods of standing or sitting. If your varicose veins are not improving, the next step may be to perform a procedure to correct the venous reflux.
Most varicose veins connect directly or through branches (tributaries) to a straighter, longer, larger, and deeper vein called saphenous vein, in a way very similar to how numerous smaller channels feed the waters of the main river. Treating varicose veins without correcting the reflux within the saphenous vein and its tributaries is similar to trimming only the tip of tree branches with the intention of taking down the whole tree. All the refluxing veins, including the saphenous, tributaries, and varicose veins must be treated at once or during separate treatment sessions. The largest veins should be treated first. For the treatment of the main trunk (saphenous vein) endovenous thermal ablation is recommended. This procedure uses laser or radiofrequency to deliver heat via a catheter to the vein lumen for the purpose of closing off the refluxing vein.
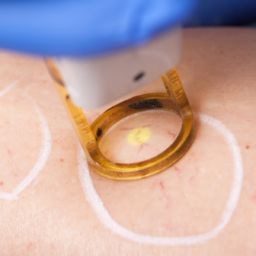
For the treatment of the tributaries and varicose veins, sclerotherapy injections are often recommended. These injections, which are performed with or without ultrasound guidance, involve injecting a solution that will cause irritation to the lining of your blood vessel, resulting in the vein collapsing and turning into scar tissue over time. Stab avulsion phlebectomies are performed usually in combination with endovenous thermal ablation and/or sclerotherapy for the treatment of the most prominent varicose veins. In this procedure, the vein specialist removes the varicose veins through multiple very small skin incisions. No stitches are needed. All our procedures are performed in the office setting using just local anesthesia. Both medical and cosmetic outcomes are excellent.
Your vein specialist can help determine which route of treatment would be best for your case. Don’t suffer through the pain, embarrassment and possible long-term problems attributed to your varicose veins any longer.
Varicose Vein Surgery
In severe cases, or cases that are not responding to conservative treatments, surgery may be required. However, with the introduction of endovenous ablation, surgery for varicose veins is rarely needed. Some common types of varicose vein surgery include vein stripping or SEPS (Subfascial Endoscopic Perferator Surgery). Your vein specialist can help determine which route of treatment would be best for your individual case.
Varicose Vein Treatment at Certified Foot & Ankle Specialists
Our staff includes an experienced vein doctor also known as a phlebologist to ensure we provide the proper diagnosis and suggest options such as noninvasive vein treatment. Don’t suffer through the pain, embarrassment, and possible long-term problems attributed to your varicose veins any longer. We specialize in the treatment of damaged veins and employ the latest procedures to get you back to enjoying the active lifestyle of South Florida without worry. When searching online for ‘varicose vein treatment near you‘ consider our locations in Broward, Palm Beach, and Martin Counties to serve you better. Make your appointment today! 1-855-550-FEET
Frequently Asked Questions About Varicose Veins
Q. How are varicose veins diagnosed?
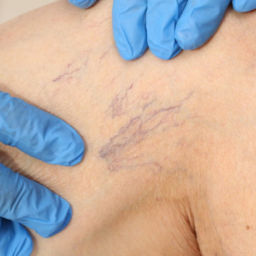
A: Varicose veins are typically diagnosed through a physical examination where your vein specialist will visually inspect your legs while you’re standing. Your doctor may also use duplex ultrasound imaging to evaluate blood flow and identify venous reflux in the affected veins. This non-invasive test helps determine the severity of the condition and guides the most appropriate treatment plan.
Q. What are the risk factors for varicose veins?
A: The most common risk factors include family history, advanced age, female gender, obesity, and occupations requiring prolonged standing or sitting. Pregnancy, hormonal changes, and previous leg injuries can also increase your risk. These factors contribute to weakening of vein walls and valves over time, leading to blood pooling and vein enlargement.
Q. How can I prevent varicose veins?
A. Prevention focuses on improving circulation through regular exercise, maintaining a healthy weight, and avoiding prolonged periods of standing or sitting. Elevating your legs when resting, wearing compression stockings if recommended, and staying hydrated can also help. While genetic predisposition cannot be changed, these lifestyle modifications can significantly reduce your risk.
Q. Can varicose veins go away naturally?
A: Varicose veins typically do not disappear on their own and tend to worsen over time without treatment. However, conservative measures like compression therapy, exercise, and leg elevation can help manage symptoms and prevent progression. Early intervention with professional treatment is recommended to prevent complications and achieve the best cosmetic and medical outcomes.
Q. When should I worry about varicose veins?
A. You should seek medical attention if you experience persistent leg pain, swelling, skin changes, or bleeding from varicose veins. Other concerning symptoms include leg ulcers, blood clots, or severe skin discoloration around the affected veins. Early treatment can prevent serious complications such as chronic wounds, deep vein thrombosis, or chronic venous insufficiency.
Q. What are the complications of untreated varicose veins?
A: Untreated varicose veins can lead to serious complications, including leg swelling, skin discoloration, chronic wounds, and blood clots. Severe cases may develop venous ulcers that are difficult to heal, superficial thrombophlebitis, or deep vein thrombosis. These complications can significantly impact your quality of life and require more extensive treatment than early-stage varicose veins.
Q. What are the most effective treatments for varicose veins?
A: The most effective treatments include endovenous thermal ablation (using laser or radiofrequency) for larger saphenous veins, and sclerotherapy injections for smaller tributaries and varicose veins. Stab avulsion phlebectomy may be used for prominent varicose veins, often combined with other treatments. These minimally invasive procedures are performed in-office with local anesthesia and provide excellent medical and cosmetic results.