What is an Ulcer?
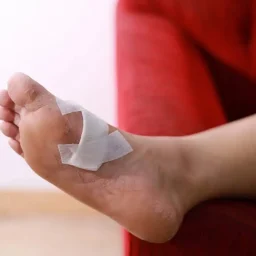
An ulcer is a breakdown in the skin, resulting in an open sore. Generally, the ulcer is round and it may have a thickened border. Ulcers may bleed, drain or cause pain and can occur anywhere on your lower extremities.
What Causes Diabetic Wounds?
- Elevated blood glucose: When blood sugars reach levels higher than 200 the immune system lowers. This can contribute to the formation of wounds. A small cut that may normally heal without problems may actually become a larger, deeper ulcer due to the dysfunction of the immune system.
- Poor circulation: A common problem in patients with diabetes, is poor circulation. Elevated sugars in the blood can damage the small blood vessels, especially the ones to the foot and toes. When your foot or toes are lacking enough blood, they do not receive proper nutrients. The skin can begin to break down and an ulcer can form. This is similar to a plant that is not receiving proper water- the ends become brown, crisp and dry out.
- Neuropathy: Another common condition that can lead to diabetic ulcers, is neuropathy. Neuropathy is a loss of sensation or feeling, typically in the toes and the feet. You may step on something sharp and not feel it. This can result in a small cut that later becomes a deep wound. If you put a lot of pressure in the same place on your foot, daily, this can also result in a special type of ulcer called a pressure ulcer.
HOW CAN I PREVENT GETTING A DIABETIC WOUND?
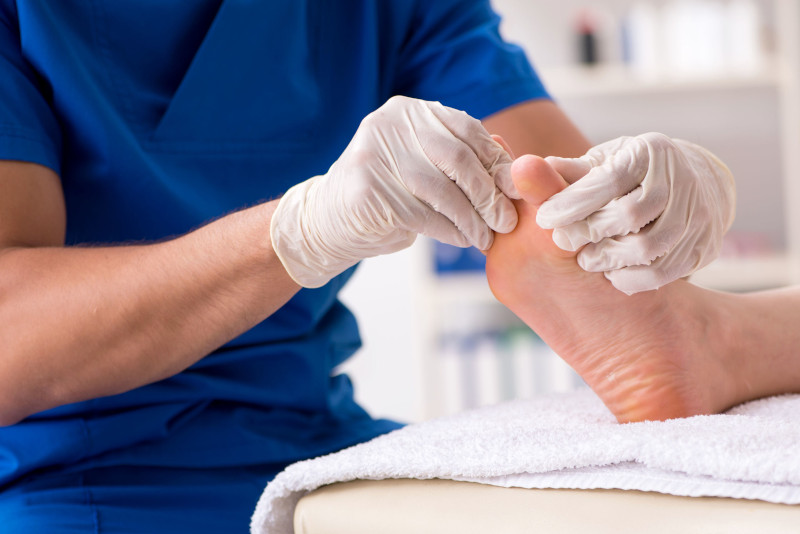
- Check your feet: Check your feet often. The best medicine is preventative medicine. Make it a habit to check your feet each night, before bed. Take care to look between the toes, check the bottoms and tops of the feet, and if you notice any unusual spot, alert your doctor right away.
- Monitor your blood glucose: If you are suffering from diabetes, make it a habit to check your blood glucose, daily. It is important to keep tabs on this number to make sure it is at a healthy range to allow for ideal immune function. Diet and exercise are a great adjunctive measure to help regulate your blood glucose.
- Watch for any new changes or pain: Pay attention to how your legs and feet feel. If you suddenly have cramping when walking, or you feel like your legs or feet are getting tired when walking, consider having your circulation checked. If you notice the hair is no longer growing on your feet or toes, this is also a sign of poor circulation. Your podiatrist can perform a simple circulation test to further evaluate your circulation.
- Pay attention if your feet or toes are numb: If you have any numbness, burning or tingling, you may be suffering from neuropathy. Make sure to never walk barefoot. When wearing socks, choose a white sock, that way if you have a bleeding wound, you can see it on your sock. Also, check your feet for any pressure sores. Your podiatrist can perform different tests to check for your nerve function.
- Appropriate shoe-wear: Wearing appropriate, well fitting shoes is an important way to help prevent the development of diabetic ulcers. You should avoid walking around barefoot. When buying new shoes, you should have your feet measured to ensure that you are wearing the most appropriate size. Make sure you try the shoes on before buying them as you may wear a slightly different size with one shoe brand versus another. Your podiatrist can also inspect and evaluate your shoewear to make sure that they are the most appropriate for you. Based on clinical findings and eligibility, diabetic shoes are also an option for diabetic patients. These shoes come in a variety of styles but, most importantly, they have extra depth and contain soft plastazote inserts. At Certified Foot and Ankle Specialists, we provide diabetic shoes with custom plastazote inserts which are very effective at protecting your feet from developing diabetic wounds.
HOW CAN I HEAL MY WOUND FASTER?
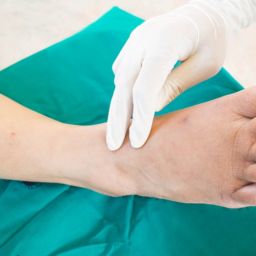
- Local wound care: Seeing your local podiatrist regularly for local wound care is critical for success in healing your ulceration. You may notice some thick yellow tissue overlying your wound, which is called fibrotic tissue or “slough” in layman’s terms. This non-viable tissue includes a biofilm that impedes wound healing. Therefore it is best to see your podiatrist on a regular basis for a “wound debridement” in the office, where that yellow slough and biofilm is removed from the wound. Basically this is a fancy way of “cleaning the wound.” Having a clean ulcer, with healthy bleeding tissue will provide the best conditions for your ulcer to heal.
- Off-loading the diabetic wound: Many diabetic wounds develop in areas that breakdown due to chronic pressure. In order to heal these wounds, you must be able to appropriately off-load these sites.This can be accomplished with padding or with a cut-out within the shoe or insert. Appropriately off-loading the affected area can also help prevent recurrence of the wound. Once the wound is healed, it is then best to be fitted for diabetic shoes and casted for custom plastozoate inserts. Within the insert, your podiatrist can be sure that pressure is being alleviated from the affected area.
- Bioengineered skin substitutes: With chronic, difficult healing diabetic wounds, there are a variety of local wound care treatment options. In recent years bioengineered skin substitutes have taken the wound care world by storm. These skin substitutes have growth factors that stimulate and promote wound healing. There are a variety of different bioengineered skin substitutes available, some of which include and are derived from porcine (pig), bovine (cow), and human skin tissue. These grafts can be applied right in the office by your podiatrist.
- Skin grafting and skin flaps: For large and difficult to heal diabetic foot wounds, split-thickness skin grafting is also an option. This involves taking a thin layer of skin from your own calf or thigh, which can be stretched and applied over your open wound. This new skin will get incorporated at the wound site leading to closure of the wound. Split-thickness skin grafting includes only taking a top layer of skin (“split-thickness”) from the calf or thigh, with deep underlying skin remaining intact (and not forming a new wound). Alternatively, your podiatrist may also consider doing a skin flap depending on the location. This may involve surgically excising the wound and then using nearby skin to manipulate and rotate over the wound site. Appropriate skin flapping technique allows for closure of the wound and surrounding skin with stitches.
- Surgical options: Besides local wound care, surgical options may be considered in an attempt to off-load and prevent recurrence of a diabetic wound. This may involve excision of prominent bone at the site or may involve correction of an underlying deformity which may have led to and/or is impeding the healing of your diabetic wound. Sometimes the best wound care is not just treating the wound itself by finding out and addressing the cause.
- Watch your diet: Diet is a commonly overlooked component in regards to wound healing. Low protein and deficiency in vitamins and nutrients, such as Vitamin C and Zinc, have been shown to decrease wound healing. It’s best to have a well-balanced diet with protein, fruit, vegetables, dairy and grains. However be sure to monitor your blood sugar. Nevertheless, without the proper nutrition, your body lacks the building blocks needed to repair your skin.
To make an appointment, click here
By Dr. Derek Pawich, DPM