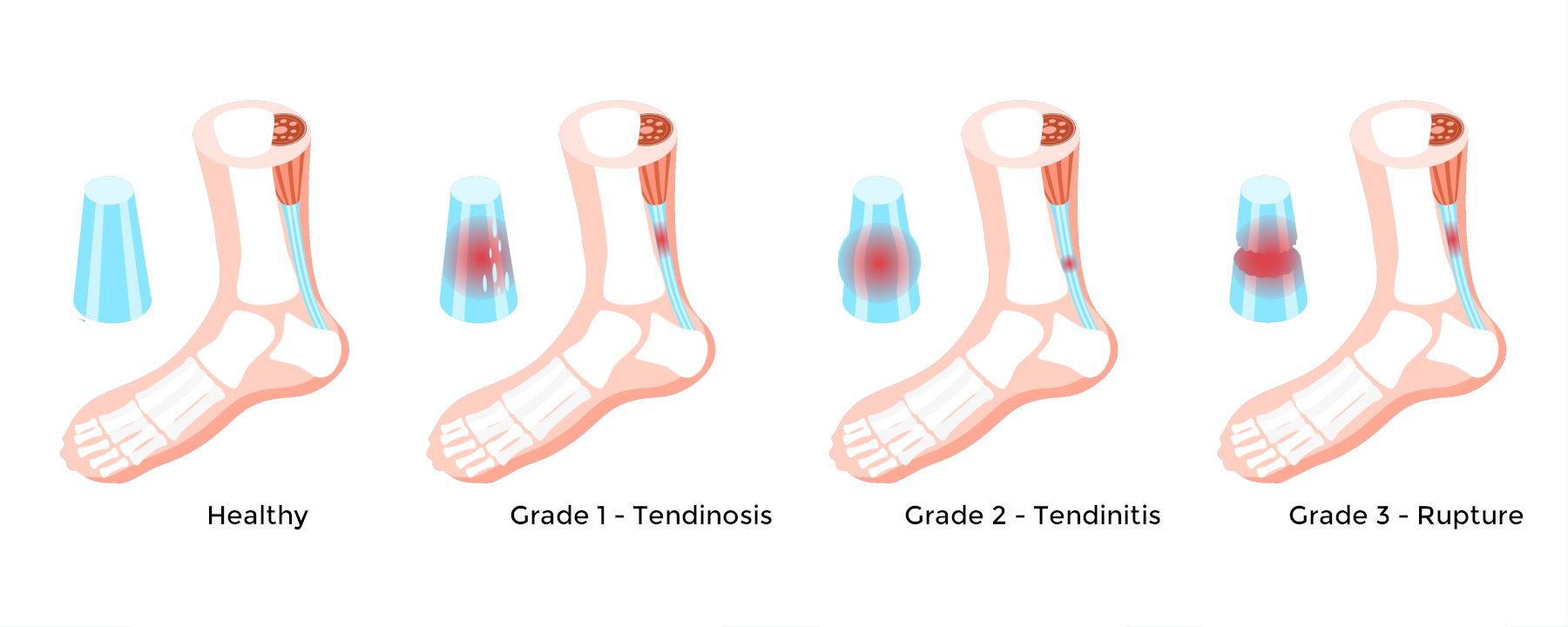
The Achilles tendon is the responsible for plantar flexion of the ankle which during walking helps to lift the heel off the ground. One of the strongest tendons in the human body is the Achilles tendon. The tendon gets blood supply from the muscle interface with the tendon, the bone interface and the peritenon (the sheath around the tendon). Therefore there is an area of the tendon approximately 2-6 cm from the heel bone that is known as the watershed area due to the lack of blood supply and is the area that is at highest risk for injury. Jobs in industries with manual labor, trauma or repeated excessive strain in a person’s daily activities can lead to an Achilles tendon rupture.
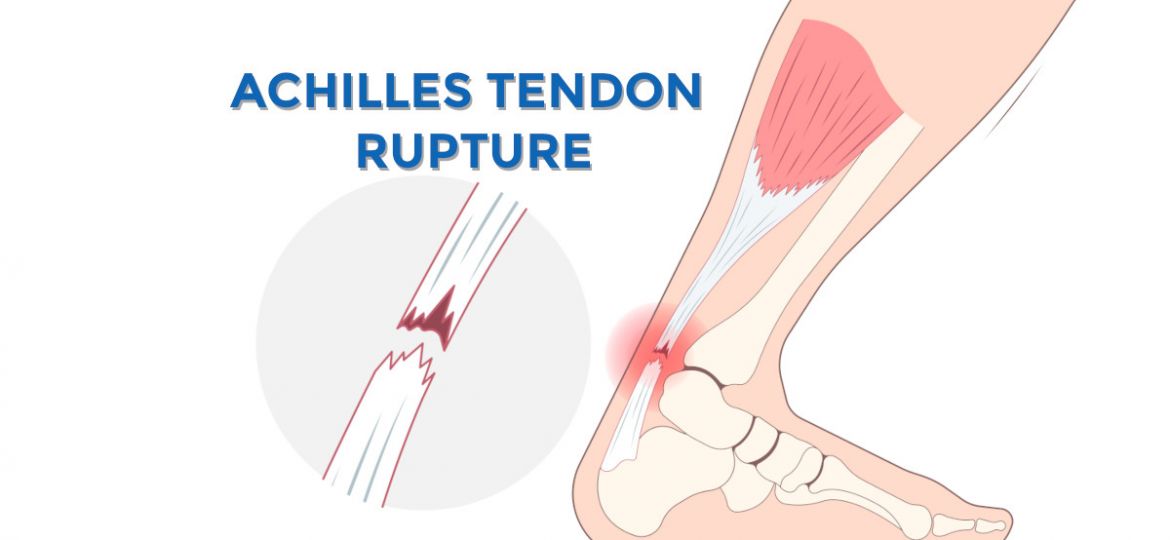
What Is An Achilles Tendon Rupture?
An Achilles rupture is a tear of the tendon at the back of the ankle and calf. The Achilles tendon is a band of tissue that connects your calf to your heel crossing the ankle joint. The reason the Achilles tendon is at risk of rupture is that there is a watershed area that has decreased blood supply and therefore places the tendon at risk of injury/rupture at this site. Achilles tendon ruptures are approximately 75% of the time in the watershed area. There can be a complete rupture of the tendon versus partial tear of the tendon. In a partial tear there are some tendon fibers still intact while a complete tear there is complete separation of the tendon ends.
How Can We Decrease The Risk of Achilles Tendon Rupture/Injuries?
Achilles tendon injuries are common especially in the athletic population but also seen in the older population. Achilles tendon ruptures have some randomness to who they affect but overall to help reduce the risk of an Achilles tendon rupture there are some recommendations. Stretching the Achilles tendon prior to activity is important and for sports/exercise it is important to warm up and cool down every time. Gradually build into activities so do not go from 0-100% but slowly build into new activities. If you are a runner, slowly increase the distance and duration of training to reduce the risk. Be aware of the surface you are exercising on and limit running on uneven surfaces. Be aware and wear appropriate and supportive shoes while performing activities.
What Are The Symptoms of Achilles Tendon Ruptures?
Symptoms of an Achilles tendon rupture vary. The most common symptom is sudden pain and swelling in the back of the calf. People describe the pain as feeling or hearing an audible pop at the back of the ankle. Some patients explain that they feel like they got hit or kicked in the back of the ankle but nothing actually did hit or kick them. Patient will notice that they are not able to push off when walking or able to plantarflex the foot down after injury.
Patients are encouraged if they experience any of these symptoms to rest, ice, elevate, and take nonsteroidal anti-inflammatories to help reduce the pain and inflammation. Patient is then encouraged to seek medical attention to have the ankle evaluated.
How Are Achilles Tendon Ruptures Diagnosed?
Achilles tendon ruptures are typically diagnosed off of clinical examination. Your doctor will evaluate clinically and can palpate the gap in the tendon in a complete tear. The doctor will also evaluate by squeezing your calf muscle and look for lack of motion at the ankle. Sometimes diagnostic imaging will be ordered most commonly an MRI of the ankle to confirm the diagnosis. An X-ray is non specific and therefore if imagining is used to confirm the diagnosis typically it is an MRI at your local podiatrist.
What Are The Complications of Achilles Tendon Ruptures?
Not all Achilles tendon rupture are diagnosed immediately. If a delay in the identification of a rupture occurs the patient risks having decreased strength and function at the ankle joint. The patient risks the tendon scarring and healing in an elongated position which can cause abnormal gait and further problems.
What Are The Treatment Options For Achilles Tendon Ruptures?
When it comes to Achilles tendon ruptures there are surgical and nonsurgical treatment options. Nonsurgical treatment is typically reserved for acutely found ruptures in patients with low activity levels, partial ruptures, medical conditions preventing them from being cleared for surgical intervention.
Nonsurgical Treatment
Casting in a plantarflexed position to allow the ruptured ends of the tendon to scar back together and then aggressive physical therapy protocol to help regain strength and activity. A nonsurgical treatment approach is associated with increased risk of re-rupture but otherwise in the literature has comparable results to surgical intervention. Nonsurgical treatment also risks the tendon healing in an elongated position and therefore having a decrease in strength of the tendon.
Surgical Options
Surgical intervention is typically recommended for complete tear of the Achilles tendon. This can be done with multiple different approaches depending on the severity of the rupture your surgeon will discuss the options and what is recommended. Treatment using a surgical method does decrease the risk of re-rupture and improves the push-off strength due to being able to control the tension applied to the repaired tendon. There are risks with surgical intervention including but not limited to infection, incision site healing issues, nerve pain, risk of re-rupture/failure of implants.
Rehabilitation and Recovery
Physical therapy is necessary in both surgical and nonsurgical treatment. Physical therapy helps reducing the scarring after surgical treatment and helps strengthen and improve range of motion after rupture. Recovery from an Achilles tendon rupture can take upwards of 6-9 months before returning fully to activities. Physical therapy is the main determinant of length of recovery and is the most important part of the recovery for regaining strength and returning to activities.
Call Our Foot And Ankle Specialists today!
If you have a ruptured achilles tendon, reach out to our staff or foot doctors located in South East and West of Florida. With convenient foot and ankle locations in Tampa, St. Petersburg, Palm Harbor and Brandon we service the Gulf Coast area of Florida.
Please contact us today at 855-550-3338 or send us a message to schedule a consultation.