Flat feet affect millions of people, causing discomfort that ranges from mild annoyance to debilitating pain. As board-certified podiatrists at Certified Foot and Ankle Specialists, we frequently help patients understand how to fix flat feet using proven treatment methods. Whether you’re dealing with fallen arches from birth or adult-acquired flat foot, effective solutions exist to restore your foot function and eliminate pain.
Key Takeaways
- Conservative treatments work for most cases: Custom orthotics, proper footwear, and targeted exercises can significantly improve flat feet symptoms without surgery
- Not all flat feet require treatment: Many people with flat arches experience no pain and need no intervention
- Early intervention prevents complications: Addressing flat feet promptly can prevent arthritis, tendon damage, and chronic pain later in life
- Multiple treatment approaches available: From simple arch supports to surgical reconstruction, treatment is customized to your severity and lifestyle needs
- Professional evaluation is essential: A podiatrist can determine whether your flat feet require treatment and recommend the most effective approach
Understanding Flat Feet (Fallen Arches)
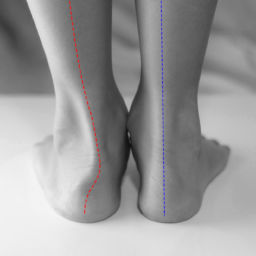
Flat feet, medically known as pes planus, occur when the arch of your foot collapses or never develops properly. In a normal foot, the arch provides natural shock absorption and helps distribute body weight evenly. When you have flat feet, your entire sole makes contact with the ground during standing and walking.
The posterior tibial tendon plays a crucial role in maintaining your arch. This tendon runs along the inside of your ankle and helps support the arch structure. When this tendon weakens or becomes damaged, adult-acquired flat foot can develop even if you had normal arches previously. We will first discuss the types and then how to fix flat feet.
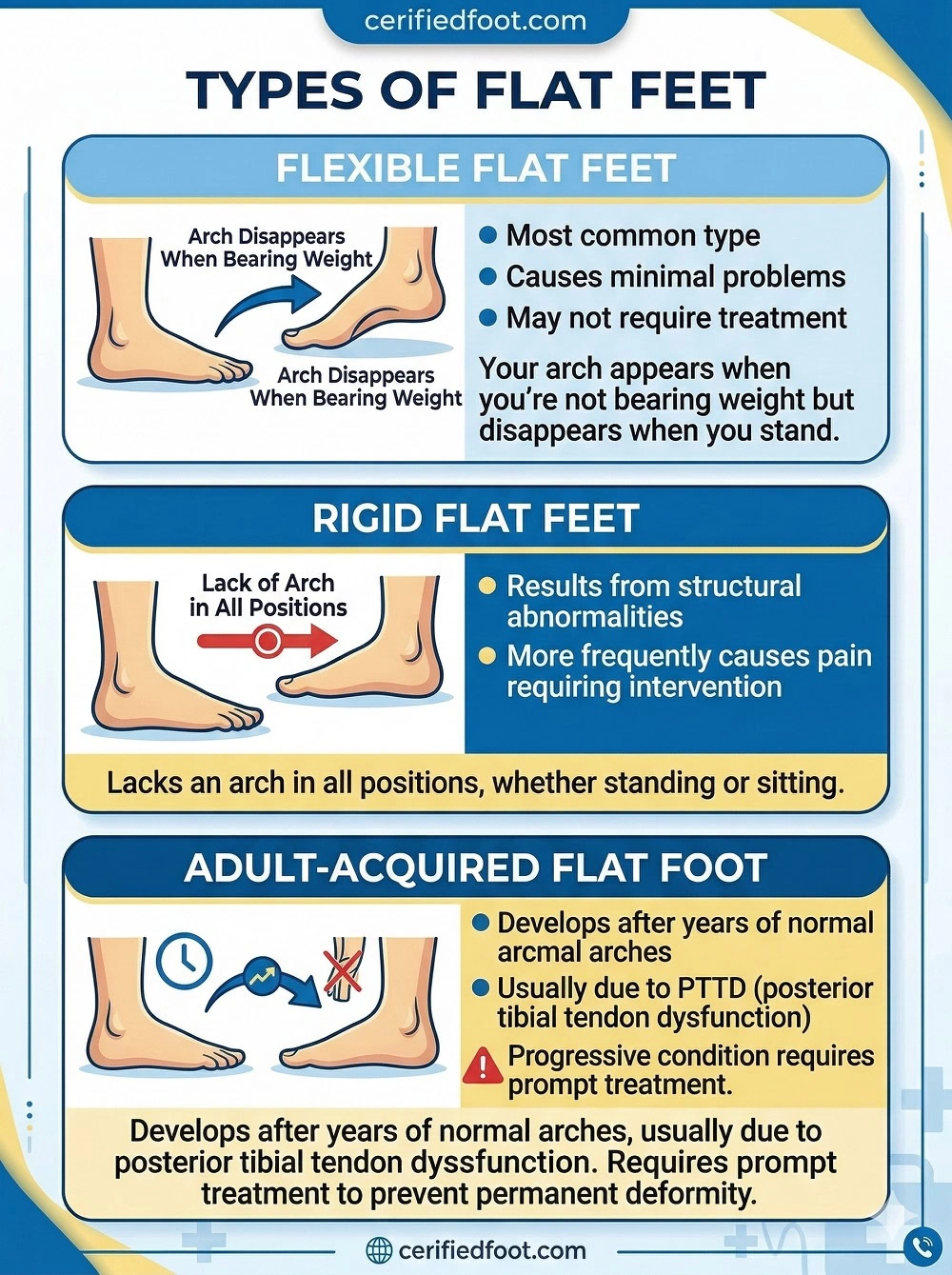
Types of Flat Feet
Flexible flat feet are the most common type. Your arch appears when you’re not bearing weight but disappears when you stand. This condition often causes minimal problems and may not require treatment.
Rigid flat feet lack an arch in all positions, whether standing or sitting. This type typically results from structural abnormalities and more frequently causes pain requiring intervention.
Adult-acquired flat foot develops after years of normal arches, usually due to posterior tibial tendon dysfunction. This progressive condition requires prompt treatment to prevent permanent deformity.
Common Causes and Risk Factors
Several factors contribute to flat feet development. Genetics plays a significant role, with flat feet often running in families. Congenital abnormalities like tarsal coalition, where foot bones fuse abnormally, can prevent proper arch formation during childhood.
In adults, posterior tibial tendon dysfunction stands as the leading cause of acquired flat feet. Obesity places extra stress on foot structures, accelerating wear and tear on the supporting tendons and ligaments. Pregnancy-related hormonal changes can temporarily weaken ligaments, sometimes leading to permanent arch collapse.
Other contributing factors include inflammatory conditions like rheumatoid arthritis, previous foot and ankle injuries, and diabetes, which affects tendon health. Understanding your specific cause helps determine the most effective treatment approach.
Recognizing Symptoms That Need Treatment
Not everyone with flat feet experiences pain. However, when symptoms develop, they typically include pain along the inside of your ankle where the posterior tibial tendon runs. You may notice heel pain or arch pain, particularly after prolonged standing or physical activities.
Swelling near the arch area often accompanies painful flat feet. Many patients report difficulty standing for long periods and pain that worsens with activity. The condition can also affect your gait, leading to compensatory changes that cause knee, hip, or lower back pain.
Progressive symptoms warrant immediate attention. Increasing pain over time, growing deformity, development of bunions or hammertoes, Achilles tendon tightness, and difficulty with physical activities all indicate the need for professional evaluation.
Non-Surgical Treatment Options
Orthotic Devices and Arch Supports
Custom orthotics represent the cornerstone of conservative flat feet treatment. These medical devices fit inside your shoes and provide the arch support your feet lack naturally. Custom orthotics redistribute pressure across your foot, reducing strain on the posterior tibial tendon and surrounding structures.
Over-the-counter arch supports may help mild cases, but custom orthotics molded specifically to your feet provide superior support for moderate to severe flat feet. We create custom orthotics using advanced imaging technology to ensure precise fit and optimal correction.
Proper Footwear Selection
Supportive shoes with firm heel counters and adequate arch support are essential for managing flat feet. Motion control or stability shoes designed specifically for flat feet help control excessive pronation during walking and running.
Avoid wearing shoes with minimal support, extremely flexible soles, or worn-out footwear. Replace athletic shoes every 300-500 miles to ensure continued support. Proper footwear works synergistically with orthotics to maximize treatment effectiveness.
Physical Therapy and Exercises On How To Treat Flat Feet
Targeted exercises strengthen the posterior tibial tendon and surrounding muscles that support your arch. Strengthening routines include calf raises, toe curls, arch-lifting exercises, and resistance band work focused on foot and ankle muscles.
Stretching exercises maintain flexibility in the Achilles tendon, calf muscles, and plantar fascia. Tight calf muscles can exacerbate flat feet symptoms, making regular stretching crucial for treatment success.
We recommend performing strengthening exercises three to five times weekly and stretching exercises daily. A structured physical therapy program provides professional guidance to ensure proper technique and progression.
Anti-Inflammatory Treatments
Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen help reduce inflammation and manage pain during acute flare-ups. Ice therapy applied for 15-20 minutes several times daily can decrease swelling and discomfort.
Rest and activity modification allow inflamed tendons to heal. This doesn’t mean complete inactivity but rather temporarily avoiding high-impact activities that aggravate symptoms while maintaining general fitness through low-impact exercises like swimming or cycling.
Surgical Solutions for How To Fix Flat Feet
Surgery becomes necessary when conservative treatments fail after six or more months, when progressive deformity continues despite treatment, or when severe pain significantly limits daily activities. Tendon rupture or significant damage also warrants surgical intervention.
Surgical Procedure Options
Tendon repair or transfer procedures restore posterior tibial tendon function by repairing damaged tissue or transferring nearby tendons to provide additional support. Osteotomy procedures involve realigning heel bones to correct foot mechanics and restore proper arch structure.
For cases with arthritis development, arthrodesis or fusion procedures stabilize painful joints. Many surgeons now utilize minimally invasive techniques that involve smaller incisions and promote faster recovery. Complex cases may require combination procedures addressing multiple structural abnormalities simultaneously.
Recovery typically requires six to twelve weeks of non-weight bearing, followed by structured physical therapy. Most patients achieve significant pain reduction and improved function, though full recovery may take several months. Our surgical team provides comprehensive pre-operative evaluation and post-operative care to optimize outcomes.
Prevention and Maintenance Strategies
Maintaining healthy body weight reduces extra stress on foot structures and decreases progression risk. Even modest weight loss can significantly decrease symptoms in overweight individuals with flat feet.
Choose low-impact exercises like swimming, cycling, or using an elliptical machine to maintain fitness while minimizing stress on your feet. Gradually return to higher-impact activities as symptoms improve, and cross-train to prevent overuse injuries.
Wear supportive shoes daily and use orthotics consistently for maximum benefit. Avoid prolonged barefoot walking on hard surfaces, which increases stress on already-compromised arch structures. Continue strengthening exercises even after symptoms improve to maintain posterior tibial tendon health.
Professional Evaluation at Certified Foot and Ankle Specialists
Our comprehensive diagnostic process begins with a thorough physical examination, gait analysis, and biomechanical assessment. We evaluate your posterior tibial tendon function, foot flexibility, and range of motion to determine the type and severity of your flat feet.
Imaging studies including X-rays reveal bone alignment and identify conditions like tarsal coalition or arthritis. When needed, MRI scans provide detailed visualization of tendon damage and soft tissue abnormalities.
We develop personalized treatment plans tailored to your specific condition severity, lifestyle requirements, and activity goals. Our staged treatment approach begins with conservative methods and progresses to advanced interventions only when necessary. Regular monitoring allows us to adjust protocols based on your response to treatment.
Conclusion
Understanding how to fix flat feet begins with professional evaluation to determine the most appropriate treatment approach for your specific condition. Conservative options including custom orthotics, proper footwear, and targeted exercises successfully manage symptoms for the majority of patients.
When conservative treatments prove insufficient, surgical solutions provide effective correction and long-term relief. Early intervention prevents complications and offers the best outcomes, making prompt professional consultation essential when symptoms develop.
At Certified Foot and Ankle Specialists, our board-certified podiatrists combine extensive experience with advanced diagnostic technologies to deliver comprehensive flat feet treatment. With multiple locations across Florida, we provide accessible, expert care to help you achieve pain-free mobility and optimal foot function.
Don’t let flat feet limit your lifestyle. Contact Certified Foot and Ankle Specialists today to schedule a thorough evaluation and discover which treatment approach can restore your foot health and quality of life.
*About the Author: Dr. Kyle J. Kinmon, MS, DPM, FACFAS
This article was reviewed by a board-certified podiatrist with over 15 years of experience in diagnosing and treating foot and ankle conditions. Our practice specializes in comprehensive foot care, from common conditions like tendonitis to complex surgical interventions.