Running with plantar fasciitis is possible for many patients, but requires proper footwear, modified training volume, and close monitoring of symptoms to avoid worsening the condition. The decision to continue running depends on pain severity, tissue healing status, and individual biomechanics.
Key Takeaways
- Can I run with plantar fasciitis? Many runners can continue with reduced mileage and proper footwear, but running through severe pain often delays recovery.
- What causes plantar fasciitis in runners? Overtraining, inadequate footwear support, tight calf muscles, and excessive pronation are the primary contributors.
- How should you modify your running? Reduce weekly mileage by 30-50%, switch to softer surfaces, and incorporate rest days between runs.
- When should you stop running completely? If pain increases during runs, persists for hours afterward, or causes limping, complete rest is necessary.
- What footwear helps plantar fasciitis? Running shoes with firm arch support, cushioned heels, and a 10-12mm heel-to-toe drop reduce plantar fascia strain.
What Is Plantar Fasciitis and How Does It Affect Runners?
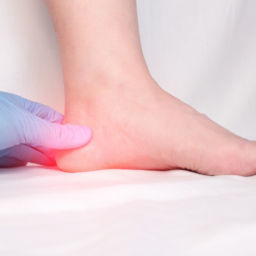
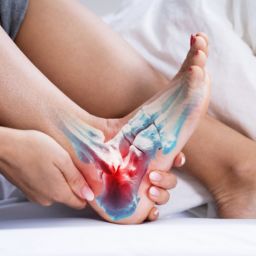
Plantar fasciitis occurs when the plantar fascia—the thick band of tissue connecting your heel bone to your toes—develops micro-tears and inflammation from repetitive stress.
The plantar fascia acts as a shock-absorbing bowstring that supports your foot’s arch during walking and running. In runners with sports-related overuse injuries, the repetitive impact of thousands of foot strikes creates cumulative stress on this tissue, particularly at its insertion point on the heel bone.
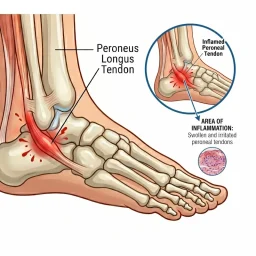
While plantar fasciitis usually targets the heel and arch, runners may also notice outer foot pain after running if they alter their gait to compensate for the discomfort. Typically, the condition manifests as sharp, stabbing sensations that are most intense during those first few morning steps or after sitting for a while. Although the pain often eases as the tissue warms up during activity, it tends to flare up again once you rest or finish a long run. So, if your heel hurts or you have outer foot pain after running, you should read what our foot doctors have to say about getting back on the track.
Most people find relief from plantar fasciitis within 6 to 18 months by sticking to basic remedies like rest, consistent stretching, and supportive shoes. While the body can sometimes heal itself over time, taking an active approach to treatment usually speeds things up, often showing noticeable improvement in just 8 to 12 weeks.
This condition affects approximately 10% of runners at some point in their training, making it one of the most common overuse injuries in the sport.
“According to the American Academy of Family Physicians, plantar fasciitis affects about 10% of the population during their lifetime and accounts for approximately 1 million patient visits per year, with an incidence of 5-10% specifically among recreational and elite runners.”
What Causes Plantar Fasciitis in Runners?
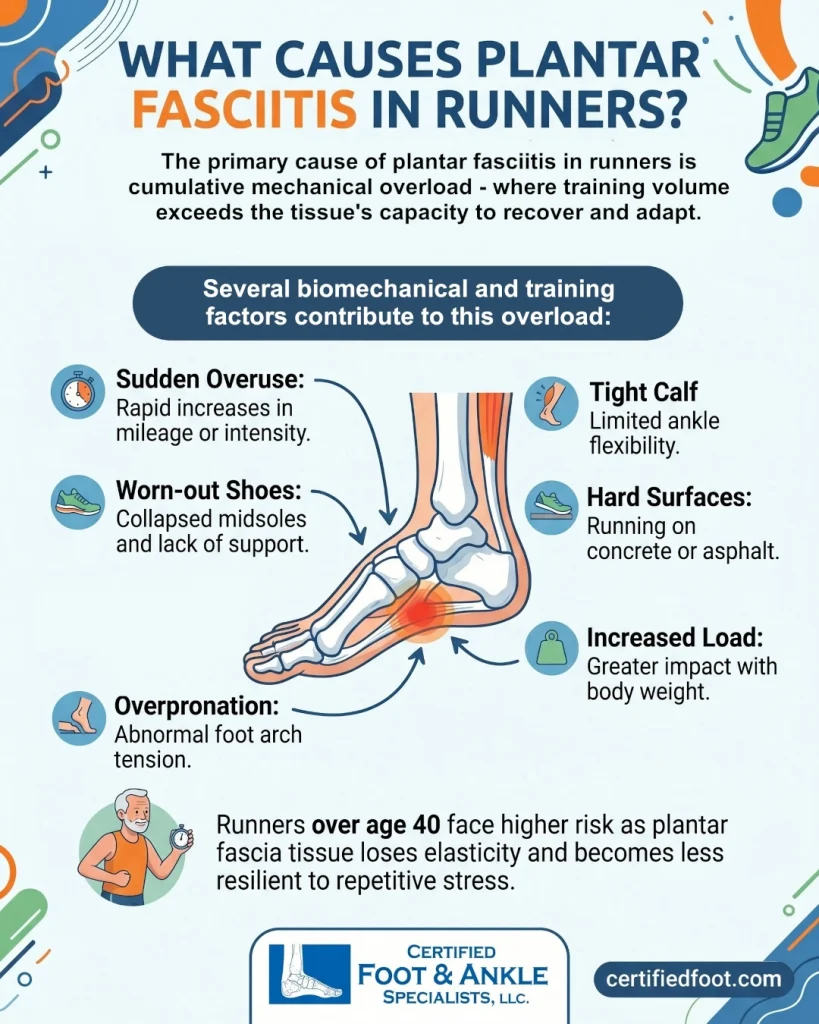
The primary cause of plantar fasciitis in runners is cumulative mechanical overload—when training volume exceeds the tissue’s capacity to recover and adapt. At that point, some patients claim their plantar fasciitis is so severe they can no longer walk.
Several biomechanical and training factors contribute to this overload:
- Training errors: Sudden increases in weekly mileage, intensity, or hill workouts without adequate progression
- Inadequate footwear: Worn-out running shoes with collapsed midsoles or insufficient arch support
- Tight calf muscles: Reduced ankle dorsiflexion increases strain on the plantar fascia during push-off
- Excessive pronation: Overpronation during the gait cycle places abnormal tension on the arch
- Hard running surfaces: Consistent training on concrete or asphalt increases impact forces
- Body weight: Carrying excess weight increases load on the plantar fascia with each foot strike
Runners over age 40 face higher risk as plantar fascia tissue loses elasticity and becomes less resilient to repetitive stress.
Can You Continue Running with Plantar Fasciitis?
Many runners can continue training with plantar fasciitis if they modify intensity, volume, and biomechanics while closely monitoring symptoms.
The decision to run should be based on pain response during and after activity. If pain remains mild (3 out of 10 or less on a pain scale), stays localized to the heel without spreading, and does not increase during the run, continuing with modifications is often appropriate.
However, you should stop running immediately if you experience worsening pain during the run, significant limping or altered gait mechanics, sharp pain that forces you to stop mid-run, or pain that persists for more than two hours after finishing.
The tissue healing timeline for plantar fasciitis typically spans 6-12 weeks with appropriate treatment. Running through severe pain extends this recovery window and increases risk of developing chronic plantar fasciitis that may take six months or longer to resolve.
“Research published in Medicine & Science in Sports & Exercise found that runners who ran more than 40 kilometers per week (approximately 25 miles) had six times higher odds of developing plantar fasciitis compared to those who ran 6-20 kilometers per week, underscoring the importance of training volume management in injury prevention and recovery.”
Conservative runners who reduce training load at the first sign of symptoms generally recover faster than those who attempt to maintain full mileage through acute pain episodes.
How Should You Modify Your Running with Plantar Fasciitis?
The most effective running modifications reduce mechanical stress on the plantar fascia while maintaining cardiovascular fitness and running-specific conditioning.
Training Volume Adjustments
- Reduce total weekly mileage by 30-50% from your current volume. If you normally run 30 miles per week, drop to 15-20 miles and monitor symptoms for two weeks before any increases.
- Eliminate speed work, tempo runs, and hill training temporarily. These high-intensity sessions place greater strain on the plantar fascia than easy-paced running.
Surface Selection
- Transition to softer running surfaces like synthetic tracks, grass fields, or dirt trails. These surfaces reduce impact forces compared to concrete sidewalks or asphalt roads.
- Avoid cambered surfaces that force one foot to pronate excessively, such as running on the shoulder of a road with a pronounced slope.
Recovery Strategies
- Schedule at least one full rest day between runs. The plantar fascia requires 24-48 hours to adapt to mechanical stress.
- Apply ice to the heel for 15 minutes immediately after each run to reduce inflammation.
- Perform calf and plantar fascia-specific stretches twice daily, holding each stretch for 30 seconds and repeating three times.
“According to Mayo Clinic physical therapists, consistently performing stretching exercises that target both the plantar fascia and Achilles tendon is critical to successful long-term treatment, as these stretches help relieve the extra stress on the plantar fascia and allow micro-tears to heal.”
Cross-Training Options
Substitute non-weight-bearing cardiovascular activities on non-running days, including swimming, pool running with a flotation vest, cycling with proper bike fit, or using an elliptical trainer.
What Are the Best Running Shoes for Plantar Fasciitis?
The ideal running shoe for plantar fasciitis provides firm arch support, adequate cushioning, and structural stability to reduce plantar fascia strain during the gait cycle.
Essential Shoe Features
- Arch support: A built-in medial arch that prevents excessive flattening during midstance
- Heel cushioning: At least 20-25mm of cushioning material in the heel stack to absorb impact forces
- Heel-to-toe drop: A 10-12mm drop reduces Achilles tendon strain and transfers less stress to the plantar fascia
- Firm midsole: Avoid shoes with excessively soft or unstable midsoles that allow excessive pronation
- Proper fit: Shoes should be replaced every 300-400 miles as midsole compression reduces support
When to Consider Custom Orthotics
Runners who do not improve with supportive shoes alone may benefit from custom orthotics. These medical-grade devices are designed from a mold of your foot and provide individualized arch support and biomechanical correction.
A board-certified podiatrist can perform a gait analysis and determine whether structural abnormalities like excessive pronation, rigid high arches, or leg length discrepancies require custom orthotic intervention.
When Should You See a Podiatrist About Plantar Fasciitis?
You should consult a board-certified podiatrist if heel pain persists for more than two weeks despite rest and home treatment, or if conservative measures fail to improve symptoms.
Immediate evaluation is warranted if you experience sudden onset of severe heel pain following trauma, significant swelling or bruising in the heel, numbness or tingling in the foot, or pain that worsens progressively despite rest.
A podiatrist will conduct a comprehensive examination including gait analysis, range of motion testing, palpation to locate the exact source of pain, and diagnostic imaging if needed to rule out stress fractures or other conditions.
Advanced Treatment Options
For cases that do not respond to conservative care, podiatrists offer several advanced interventions. These include custom orthotics for biomechanical correction, night splints to maintain a gentle stretch, corticosteroid injections, extracorporeal shockwave therapy, and platelet-rich plasma injections.
Surgical intervention is reserved for severe cases that fail to improve after 6-12 months of conservative treatment and involves partial release of the plantar fascia from the heel bone.
How Can You Prevent Plantar Fasciitis When Running?
The most effective prevention strategy is gradual training progression—increasing weekly mileage by no more than 10% per week and allowing adequate recovery between hard efforts.
“The American College of Foot and Ankle Surgeons identifies training errors—particularly sudden increases in weekly mileage or intensity without adequate progression—as a primary mechanical risk factor for plantar fasciitis, supporting the widely recognized 10% weekly increase guideline used by sports medicine professionals.”
Injury Prevention Checklist for Runners
- Perform daily calf and foot stretching, especially before morning runs
- Replace running shoes every 300-400 miles or when midsole compression is visible
- Incorporate strength training for foot intrinsic muscles and lower leg stabilizers
- Maintain a healthy body weight to reduce mechanical load on feet
- Vary running surfaces throughout the week to distribute impact forces differently
- Avoid running in minimalist shoes or barefoot if you have a history of plantar fasciitis
Runners who consistently follow these prevention principles reduce their plantar fasciitis risk by approximately 70% compared to those who make sudden training changes or neglect recovery practices.
Conclusion
Running with plantar fasciitis requires a balanced approach that respects tissue healing timelines while maintaining fitness. The key is early intervention—reducing training volume at the first sign of heel pain prevents minor inflammation from progressing to chronic injury.
If you’re experiencing persistent heel pain that interferes with running or daily activities, our board-certified podiatrists at Certified Foot and Ankle Specialists provide comprehensive treatment for plantar fasciitis at locations throughout Florida, including Boca Raton, West Palm Beach, Boynton Beach, and Stuart. Contact us to schedule an appointment with a foot specialist near you.
*About the Author: Dr. Ashley Bowles ,DPM, FACFAS
Reviewed by Certified Foot and Ankle Specialists Team
Dr. Ashley Bowles is a board-certified podiatrist with over 15 years of experience treating sports injuries and foot conditions at Certified Foot and Ankle Specialists. As a Fellow of the American College of Foot and Ankle Surgeons (FACFAS), Dr. Bowles specializes in helping active patients and athletes manage injuries while maintaining their fitness goals.
Frequently Asked Questions About Running With Plantar Fasciitis
Q: Is it OK to run through plantar fasciitis?
A: It depends on pain severity. Running through plantar fasciitis is acceptable when pain stays at 3 out of 10 or below, remains localized to the heel, and does not worsen during the run. If pain escalates mid-run, causes limping, or persists for more than two hours after finishing, running should stop until symptoms subside. Mild cases with appropriate modifications — reduced mileage, softer surfaces, supportive footwear — generally do not cause permanent damage. Severe or worsening pain that is ignored significantly increases the risk of developing chronic plantar fasciitis.
Q: How long does plantar fasciitis last in runners?
A: Most runners see meaningful improvement within 6 to 12 weeks with consistent treatment, including stretching, footwear modifications, and reduced training volume. Full recovery, however, can take 6 to 18 months depending on severity, how early treatment begins, and whether the runner continues to train through significant pain. Runners who address symptoms early and reduce mechanical load on the plantar fascia consistently recover faster than those who delay treatment. Cases that remain untreated or are repeatedly aggravated by high-mileage training can become chronic, extending recovery well beyond a year.
Q: Can plantar fasciitis heal while still running?
A: Yes, plantar fasciitis can heal while running, but only under the right conditions. The plantar fascia requires reduced mechanical stress to repair micro-tears — which means continuing to train at the same volume, intensity, and surface type that caused the injury will prevent healing. Runners who successfully recover while staying active typically cut weekly mileage by 30 to 50 percent, eliminate speed work and hill training, switch to softer surfaces, and perform daily stretching. Running on a healing plantar fascia is possible; running without any modifications is not.
Q: What stretches should I do before running with plantar fasciitis?
A: Before running with plantar fasciitis, perform these three stretches to reduce morning stiffness and prepare the tissue for impact. First, the seated towel stretch: loop a towel around the ball of your foot and gently pull it toward you while keeping your leg straight, holding for 30 seconds and repeating three times. Second, the standing calf stretch: place both hands flat against a wall, step the affected foot back, press the heel firmly into the floor, and lean forward until you feel a stretch in the calf — hold 30 seconds, repeat three times per side. Third, plantar fascia massage: roll a frozen water bottle or golf ball along the arch of the foot for two to three minutes before standing. These stretches are most effective when performed before your first steps of the day and again immediately before heading out for a run.
Q: Does running make plantar fasciitis permanent?
A: Running alone does not make plantar fasciitis permanent, but consistently running through moderate to severe pain without modification can lead to chronic plantar fasciitis that is significantly harder to treat. Chronic cases develop when the plantar fascia is repeatedly stressed before adequate healing can occur, causing scar tissue buildup and structural changes to the tissue over time. Runners who modify training load early, use appropriate footwear, and follow a structured recovery plan rarely develop permanent complications. Surgical intervention is only considered after 6 to 12 months of failed conservative treatment and is uncommon — the vast majority of cases resolve fully with proper management.
Q: When should you see a podiatrist about plantar fasciitis?
A: Consult a board-certified podiatrist if heel pain persists for more than two weeks despite rest and home treatment. Seek immediate evaluation if you experience sudden onset of severe heel pain following trauma, significant swelling or bruising in the heel, numbness or tingling in the foot, or pain that worsens progressively despite rest. A podiatrist can provide advanced treatments including custom orthotics, night splints, corticosteroid injections, and shockwave therapy.
Q: How can you prevent plantar fasciitis when running?
A: The most effective prevention is gradual training progression—increase weekly mileage by no more than 10% per week. Perform daily calf and foot stretching especially before morning runs. Replace running shoes every 300-400 miles. Incorporate strength training for foot intrinsic muscles and lower leg stabilizers. Maintain a healthy body weight and vary running surfaces throughout the week to distribute impact forces differently.