Peroneal tendonitis is inflammation of the two peroneal tendons that run along the outer ankle, causing pain, swelling, and instability on the side of the foot. Most cases resolve with peroneal tendonitis conservative care treatment within six to eight weeks, but the right approach depends on severity and how quickly you act.
Key Takeaways
- What is peroneal tendonitis? Inflammation of the peroneal tendons along the outer ankle, usually caused by repetitive overuse or a sudden increase in activity load.
- What causes it? Repetitive running or jumping, worn-out footwear, high arches, ankle instability, or a sudden spike in physical activity.
- How is it treated? First-line treatment is rest, ice, compression, and anti-inflammatory medication—followed by physical therapy and an ankle brace if needed.
- When should I see a podiatrist? If outer ankle pain persists beyond two weeks, worsens with rest, or limits your ability to bear weight, get a professional evaluation.
- Can it be prevented? Yes—gradually increase training load, wear supportive footwear, and address ankle instability before symptoms develop.
What Is Peroneal Tendonitis?
Peroneal tendonitis is inflammation of the peroneus longus and peroneus brevis tendons, which stabilize the ankle and control foot eversion. These tendons run behind the outer ankle bone (the lateral malleolus) and are stressed every time your foot pushes off the ground. Unlike acute tendon tears, peroneal tendonitis develops gradually from repetitive overuse. Athletes who run, play basketball, or hike on uneven ground are especially vulnerable. However, adults over 40 often develop it from everyday activities—particularly those with high arches or a history of ankle sprains. The condition is frequently misdiagnosed as a lateral ankle sprain because the pain location overlaps. A podiatrist can distinguish the two through physical examination and imaging when necessary.
What Causes Peroneal Tendonitis?
Peroneal tendonitis results from repetitive stress that exceeds the tendon’s ability to recover. The most common trigger is a sudden increase in running mileage or intensity without adequate conditioning.
Activity & Lifestyle Causes |
Structural & Medical Causes |
|---|---|
| Sudden increase in training mileage or intensity | High arches or flat feet that strain the peroneal tendons |
| Wearing worn-out or unsupportive footwear | Previous ankle sprains that weakened tendon support |
| Running on uneven or cambered surfaces | Ankle instability from ligament laxity |
| Tight calf muscles or limited ankle flexibility | Inflammatory conditions such as rheumatoid arthritis |
In our South Florida foot and ankle clinics, we frequently see peroneal tendonitis in runners who increase weekly mileage too quickly, walkers transitioning to trail surfaces, and adults who develop it after minor ankle sprains that were never fully rehabilitated.
What Are the Symptoms of Peroneal Tendonitis?
The defining symptom is pain and tenderness along the outer ankle, directly behind or below the lateral malleolus. This tendon pain typically worsens with activity and may ease with rest in early stages—but becomes more persistent as the condition progresses.
Watch for these symptoms of peroneal tendonitis:
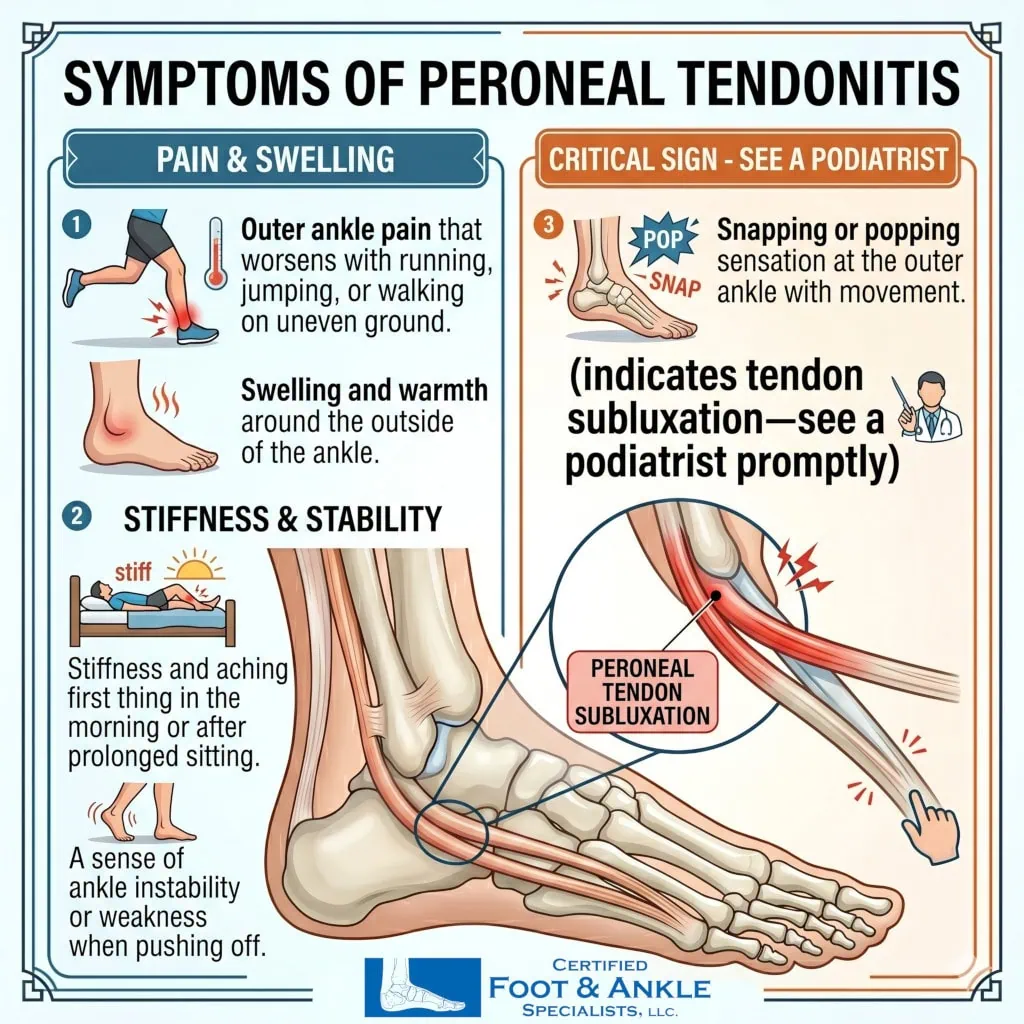
- Outer ankle pain that worsens with running, jumping, or walking on uneven ground
- Swelling and warmth around the outside of the ankle
- Stiffness and aching first thing in the morning or after prolonged sitting
- A sense of ankle instability or weakness when pushing off
- Snapping or popping sensation at the outer ankle with movement (indicates tendon subluxation—see a podiatrist promptly)
Symptoms that don’t improve within two weeks, or that worsen despite rest, are a clear signal to seek professional evaluation. Untreated peroneal tendonitis can progress to partial or complete tendon tears.
How is peroneal tendonitis different from an ankle sprain?
Peroneal tendonitis and lateral ankle sprains cause pain in the same location, but they involve different structures and require different treatment approaches. An ankle sprain damages the ligaments that connect bones at the joint. Peroneal tendonitis is inflammation of the tendons that run alongside those ligaments. The distinction matters because sprains typically involve a specific twisting incident and bruising, while tendonitis develops gradually from repetitive overuse without a clear injury event.
A key clinical test: tenderness directly over the peroneal tendons behind the lateral malleolus points to tendonitis. Tenderness over the anterior talofibular ligament (ATFL) — slightly forward on the outer ankle — suggests a sprain. Imaging confirms when the physical exam is inconclusive.
How Is Peroneal Tendonitis Treated?
Treatment for peroneal tendonitis follows a staged approach: reduce acute inflammation first, then restore strength and mobility, then address the underlying cause to prevent recurrence.
Conservative Treatments (Weeks 1–4)
The majority of peroneal tendonitis cases respond to conservative treatment when caught early. These are the initial steps our specialists recommend:
- Rest and activity modification. Reduce or pause activities that aggravate tendon pain. This doesn’t mean complete immobility—gentle movement is encouraged—but avoid running, jumping, and lateral cutting movements until pain subsides.
- Rest, ice, compression, elevation (RICE). Apply an ice pack to the outer ankle for 15–20 minutes, three to four times daily during the acute phase. Compression bandaging and elevation reduce swelling.
- Anti-inflammatory medication. Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen reduce pain and inflammation. Use as directed and consult your physician if you have contraindications.
- Ankle brace or supportive taping. A lateral ankle brace or kinesiology tape offloads the peroneal tendons and provides stability during daily activity and early return to exercise.
- Footwear correction. Replace worn-out shoes. For high arches or overpronation, a structured athletic shoe with lateral support reduces strain on the peroneal tendons.
Physical Therapy (Weeks 3–8)
Physical therapy is the backbone of peroneal tendonitis recovery. A structured program focuses on three areas: eccentric strengthening of the peroneal muscles, restoring full range of motion at the ankle, and improving proprioception (balance and joint position sense) to reduce re-injury risk.
Expect exercises to include ankle eversion strengthening with resistance bands, single-leg balance work, and progressive return-to-activity protocols. Our specialists coordinate directly with physical therapists to ensure the program matches each patient’s activity goals.
Advanced Treatment Options
When conservative treatments do not achieve adequate pain relief after six to eight weeks, additional interventions are available:
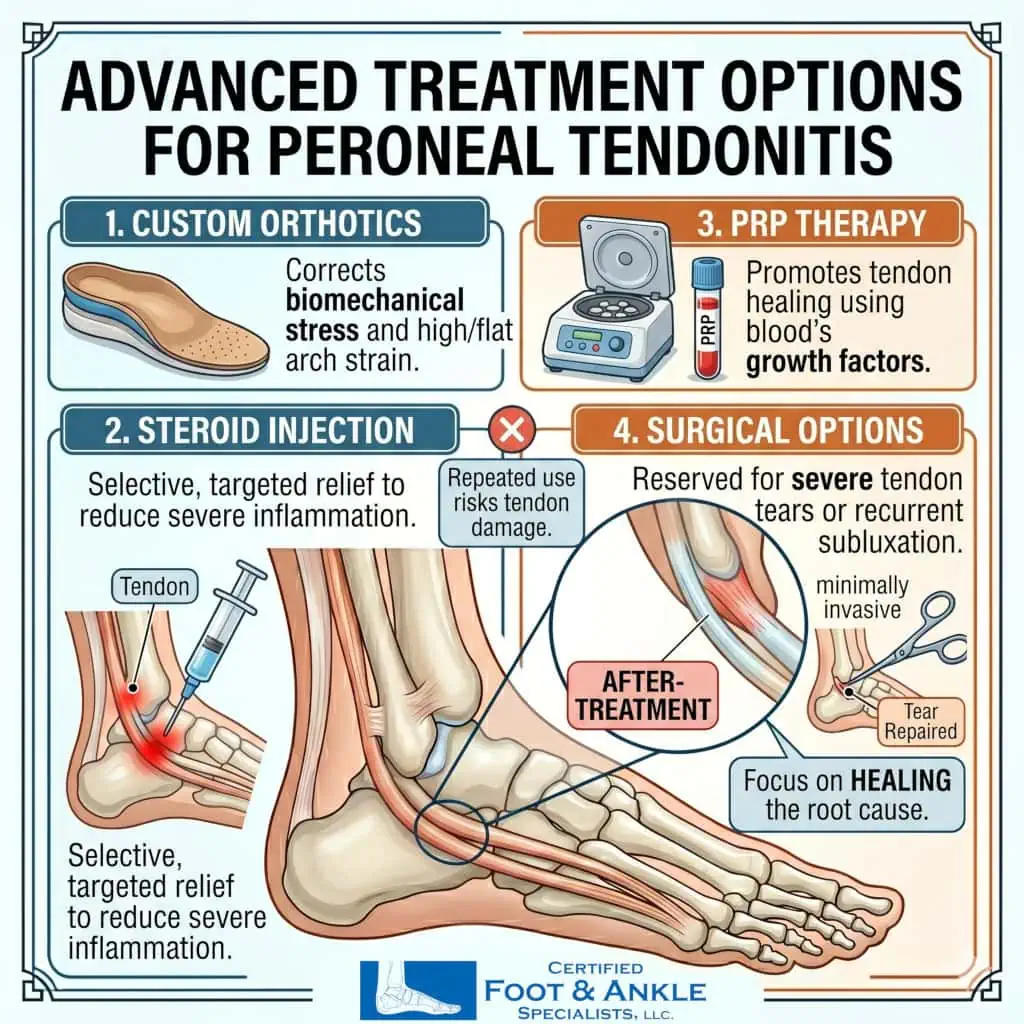
- Custom orthotics: For patients with high arches, flat feet, or chronic ankle instability, custom orthotic devices correct biomechanical stress on the peroneal tendons—addressing the root cause rather than just the symptoms.
- Corticosteroid injection (cortisone shots): A targeted injection reduces severe inflammation when conservative care stalls. This is used selectively—repeated injections near tendons carry risks and are not a long-term solution.
- Platelet-rich plasma (PRP) therapy: PRP uses your own blood’s growth factors to promote tendon healing. Evidence supports its use for chronic, treatment-resistant tendonitis.
- Immobilization boot: In moderate-to-severe cases with significant tendon damage, a walking boot allows the tendon to heal while maintaining mobility.
- Surgery: Reserved for tendon tears or cases with tendon subluxation that do not respond to non-surgical management. Minimally invasive techniques are preferred when surgical repair is required.
When Should You See a Podiatrist for Outer Ankle Pain?
See a foot and ankle specialist if outer ankle pain persists beyond two weeks despite rest and home care. Waiting too long is the most common reason peroneal tendonitis becomes a chronic, harder-to-treat problem.
Seek prompt evaluation if you experience any of the following:
- Pain that does not improve—or worsens—with rest
- Inability to bear weight on the affected foot
- Visible ankle swelling that increases over 48 hours
- A snapping or popping sensation at the outer ankle with movement
- Numbness, tingling, or significant bruising around the ankle
- A history of ankle sprains with recurring instability
Our podiatrists at Certified Foot and Ankle Specialists can confirm the diagnosis with physical examination and imaging, rule out tendon tears or stress fractures, and develop a treatment plan calibrated to your activity level and recovery goals.
How Can You Prevent Peroneal Tendonitis From Recurring?
Peroneal tendonitis has a high recurrence rate when the underlying cause isn’t addressed. Prevention requires consistent attention to load management, footwear, and ankle strength.
- Increase training load gradually. Follow the 10% rule—don’t increase weekly mileage or intensity by more than 10% per week. This gives tendons time to adapt.
- Replace footwear regularly. Athletic shoes lose structural support after 300–500 miles. Running in worn-out shoes is one of the most common preventable causes of tendon injuries.
- Strengthen your ankles. Regular peroneal strengthening exercises—ankle eversion with a resistance band, single-leg balance—maintain the tendon support system. Ask your physical therapist for a maintenance program.
- Address ankle instability. Recurrent ankle sprains weaken the lateral support structures and overload the peroneal tendons. Custom orthotics or a structured rehabilitation program can correct this before it causes tendonitis.
- Warm up before activity. Five minutes of dynamic ankle mobility work before running or sport reduces tendon strain at cold start.
The Bottom Line on Peroneal Tendonitis Treatment
Most cases of peroneal tendonitis resolve fully with conservative care—but only when treatment starts early and the root cause is corrected. Rest and ice manage the acute phase; physical therapy and footwear correction prevent recurrence. Skipping either step is why so many patients end up back in our office months later.
If outer ankle pain has lasted more than two weeks, or you’ve dealt with recurring ankle issues, don’t manage it alone. Our board-certified podiatrists at Certified Foot and Ankle Specialists treat peroneal tendonitis at locations across South Florida, including Boca Raton, West Palm Beach, Boynton Beach, Coral Springs, Delray Beach, and more. Contact us to schedule an evaluation with a foot specialist near you.
*About the Author: Dr. Kyle J. Kinmon, MS, DPM, FACFAS
This article was reviewed by a board-certified podiatrist with over 15 years of experience in diagnosing and treating foot and ankle conditions. Our practice specializes in comprehensive foot care, from common conditions like tendonitis to complex surgical interventions.
Frequently Asked Questions About Peroneal Tendonitis Treatment
Q: What is peroneal tendonitis?
A: Peroneal tendonitis is inflammation of the peroneus longus and peroneus brevis tendons, which run along the outer ankle and stabilize the foot during movement. It causes pain, swelling, and tenderness on the outside of the ankle, typically worsened by activity. The condition usually develops gradually from repetitive overuse rather than a single injury.
Q: What are the symptoms of peroneal tendonitis?
A: Symptoms of peroneal tendonitis include pain and tenderness along the outer ankle, swelling behind or below the lateral malleolus, morning stiffness, and a sense of ankle instability. Pain typically worsens with running, jumping, or walking on uneven ground, and may ease with rest in early stages. A snapping sensation at the outer ankle may indicate tendon subluxation, which requires prompt evaluation.
Q: How is peroneal tendonitis treated?
A: Peroneal tendonitis treatment starts with rest, ice, compression, and anti-inflammatory medication to manage acute inflammation. An ankle brace and footwear correction are added to reduce tendon stress during recovery. Physical therapy follows to rebuild peroneal strength and ankle stability. For cases that do not respond to conservative care within six to eight weeks, options include custom orthotics, corticosteroid injection, PRP therapy, or, rarely, surgery.
Q: How long does peroneal tendonitis take to heal?
A: Mild to moderate peroneal tendonitis typically heals within six to eight weeks with consistent conservative treatment. More severe cases or those involving tendon tears may require three to six months of rehabilitation. Returning to full physical activity too soon is the most common cause of recurrence, so a gradual, guided return-to-activity plan is essential.
Q: When should I see a podiatrist for outer ankle pain?
A: See a podiatrist if outer ankle pain persists beyond two weeks despite rest and home care, worsens with activity, or limits your ability to bear weight. Prompt evaluation is also warranted if you experience a snapping sensation at the ankle, significant swelling, numbness, or a history of recurring ankle sprains. Early diagnosis prevents peroneal tendonitis from progressing to a tendon tear.
Q: How much does peroneal tendonitis surgery cost in Florida?
A: The cost of peroneal tendonitis surgery in Florida can vary widely depending on several factors, including the specific procedure performed, the severity of the condition, the surgical facility, anesthesia fees, and your insurance coverage. Because each case is different, it’s not possible to provide an accurate estimate without an individual evaluation. Many insurance plans may cover surgery when it is deemed medically necessary, but out-of-pocket costs will depend on your specific benefits. The best way to understand your expected costs is to schedule a consultation, where a personalized treatment plan and cost breakdown can be provided. Note: This information is for general educational purposes and should not be considered a cost estimate.
Q: Can peroneal tendonitis be prevented?
A: Yes, peroneal tendonitis can largely be prevented by gradually increasing training load, replacing worn athletic shoes regularly, and performing ankle strengthening exercises. Addressing ankle instability after sprains is particularly important, as chronic instability overloads the peroneal tendons and significantly raises recurrence risk.