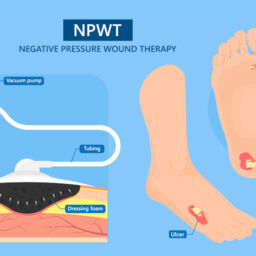
One of the major complications with infected ulcerations, especially in diabetics, is lower extremity amputation. There are about 82,000 non-traumatic leg amputations performed in the US per year in diabetic patients, representing about 60% of all nontraumatic leg amputations performed.
Appropriate wound care is imperative in preventing leg amputations. Limb salvage is a major goal in podiatry as studies have shown the debilitating effects of leg amputation. Removing a leg has a negative impact on your entire body as it results in the body requiring more energy to function. Basically, the rest of your body has to make up for that lost limb.
Adequate Blood Flow
The vast majority of leg amputations occurred in patients who had poor blood flow to their feet. Adequate blood flow is imperative to the healing of wounds. Blood flow is assessed upon your first visit to your podiatrist’s office. At Certified Foot and Ankle Specialists, we can measure your blood flow right on site. If blood flow is found to be inadequate, particularly in regards to healing your wound, then we will refer you to a vascular specialist for further intervention. Podiatrists work hand in hand with vascular surgeons to ensure proper wound healing.
Diet
Diet is a commonly overlooked component in regard to wound healing. Low protein and deficiency in vitamins and nutrients, such as Vitamin C and Zinc, have been shown to decrease wound healing. It’s best to have a well-balanced diet with protein, fruit, vegetables, dairy, and grains. However, be sure to monitor your blood sugar. Nevertheless, without the proper nutrition, your body lacks the building blocks needed to repair your skin.
Managing Blood Sugar
When blood sugar reaches levels higher than 200 the immune system decreases in function. This can contribute to the formation of wounds. A small cut that may normally heal without problems may become a larger, deeper ulcer due to the dysfunction of the immune system. High blood sugars also make it much more difficult to heal the wound and can lead to infection.
Local Wound Care
Seeing your local podiatrist regularly for local wound care is critical for success in healing your ulceration. You may notice some thick yellow tissue overlying your wound, which is called fibrotic tissue or “slough” in layman’s terms. This non-viable tissue includes a biofilm that impedes wound healing. Therefore it is best to see your podiatrist on a regular basis for a “wound debridement” in the office, where that yellow slough and biofilm is removed from the wound. Basically, this is a fancy way of “cleaning the wound”. Having a clean ulcer, with healthy bleeding tissue will provide the best conditions for your ulcer to heal.
Off-Loading the Diabetic Wound
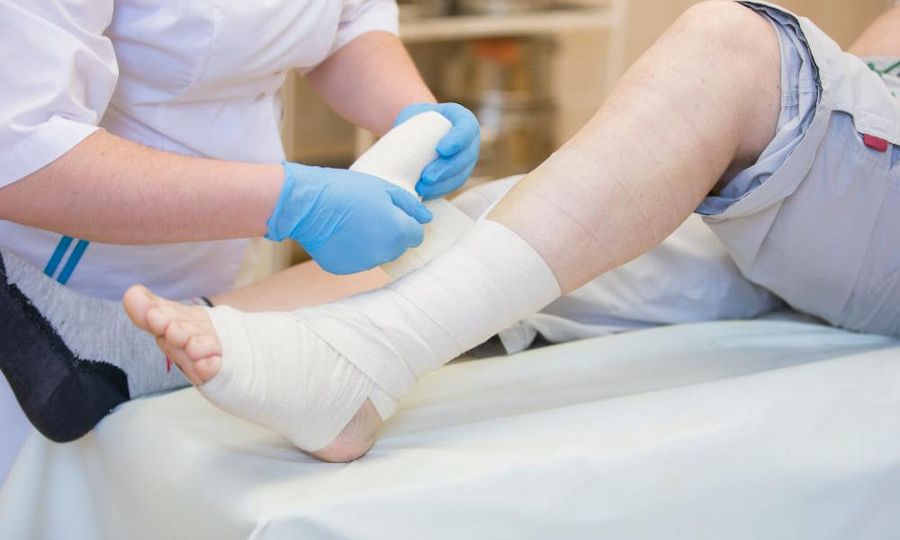
Many diabetic wounds develop in areas that break down due to chronic pressure. In order to heal these wounds, you must be able to appropriately off-load these sites. This can be accomplished with padding or with a cut-out within the shoe or insert. Soft cast applications (unna boot) can also be applied with built-in padding to effectively off-load the wounds. Appropriately off-loading the affected area can also help prevent the recurrence of the wound. Once the wound is healed, it is then best to be fitted for diabetic shoes and casted for custom plastozoate inserts. Within the insert, your podiatrist can be sure that pressure is being alleviated from the affected area.
Wound Infections
Open wounds are at great risk for developing infections, which is why you should have your wound closely followed by your podiatrist. Antibiotics are the first line of defense against infections. When an infection is suspected, cultures are taken to determine which “bug” is causing the infection and are used to ensure that you are on the most appropriate antibiotic. The longer the wound is open, the more likely it will eventually get infected. If the wound continues to get deeper and larger, it could even lead to infection in the bone thereby increasing the risk of amputation.
Surgery Options to Avoid Leg Amputation
Depending on the situation, sometimes healthy, non-infected wounds can be closed with skin grafts and skin flaps. However, surgery may be indicated to prevent limb loss. These types of surgeries are within the realm of “limb salvage” and are typically performed in a hospital setting. An example would be an “incision and drainage” where the wound is debrided in the OR and infectious material is surgically removed and washed out. However, in more severe cases, the infection can extend down to bone.
Sometimes we can address bone infection with 6 weeks of IV antibiotics, however other times partial amputation may need to be considered. There are instances where a toe amputation or even a midfoot amputation (all the toes are removed) may be indicated. Losing any sort of body part is not ideal, however, it is much less debilitating to deal with a toe amputation versus a leg amputation. Adjustments in shoewear, such as fillers, can accommodate for such amputations. Furthermore, smaller amputations, such as a toe amputation, results in much less strain on your body compared to a leg amputation. These patients are typically able to go back to living their regular lives.
Conclusion
Overall comprehensive wound care is imperative to preventing leg amputation. Adequate blood flow, diet, managing diabetes along with regular local wound care promote wound healing. The longer the wound remains open, the greater the risk of infection. Therefore, regular follow-up and wound management with your podiatrist is very important in the healing of your wound and thereby preventing amputation.
By Dr. Derek Pawich, DPM
Certified Foot and Ankle Specialist – Fort Myers, Florida