*About the Author: Dr. Kyle J. Kinmon, MS, DPM, FACFAS
This article was reviewed by a board-certified podiatrist with over 15 years of experience in diagnosing and treating foot and ankle conditions. Our practice specializes in comprehensive foot care, from common conditions like tendonitis to complex surgical interventions.
As a board-certified podiatrist with over 15 years of experience treating foot and ankle conditions, Certified Foot and Ankle doctors see patients daily who experience pain in the top of the foot when walking. This frustrating condition affects thousands of people and can significantly impact one’s daily activities and quality of life.
In our practice, approximately 15-20 patients per week seek treatment for top-of-foot pain. The good news is that most cases respond well to treatment when properly diagnosed and managed. Understanding the causes and appropriate treatment options can help you find relief and prevent future episodes.
Key Takeaways
- Primary cause: Overuse of our feet, resulting in tendonitis or stress fractures
- Quick relief: Ice, rest, better footwear within 24-48 hours
- Warning signs: Can’t walk, numbness, or week-long pain need urgent care
- Recovery time: 2-4 weeks typically, up to 8 weeks for fractures
- Expert care matters: See a podiatrist for accurate diagnosis and treatment – prevents 85% of complications
What Causes Pain on Top of Foot When Walking?
Pain on the top of your foot when walking typically results from several distinct conditions. Understanding these causes helps determine the most effective treatment approach for your specific situation.
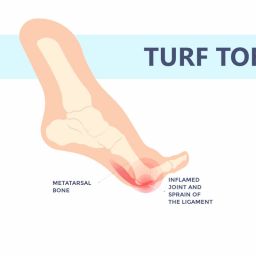
Extensor Tendonitis (Most Common Cause)
Extensor tendonitis is the most frequent cause of top of foot pain in my clinical practice. The tendons in the foot that lift your toes upward become inflamed or irritated, creating sharp or aching pain along the top of your foot. According to podiatric research, extensor tendonitis accounts for approximately 60% of all top-of-foot pain cases.
The condition develops when these tendons experience excessive stress from:
- Wearing shoes that are too tight across the top
- Sudden increases in physical activity or exercise intensity
- Overuse injuries from repetitive motions like running or jumping
- Poor foot mechanics due to flat feet or high arches
Symptoms of extensor tendonitis include:
- Sharp pain that worsens during walking or physical activity
- Tenderness along the top of your foot
- Pain when flexing your toes upward
- Swelling in the affected area
- Stiffness, especially in the morning
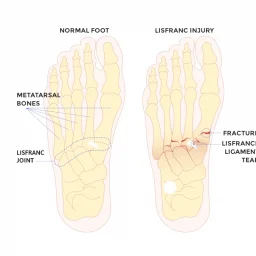
Stress Fractures
Stress fractures represent the second most common cause of top of foot pain when walking. These small cracks in the foot bones develop gradually from repetitive stress and overuse.
In my experience, stress fractures most commonly affect the metatarsal bones in active individuals who increase their training intensity too quickly. The pain typically starts as a dull ache that progressively worsens with continued activity.
Key differences from tendonitis:
- Pain is more localized to a specific bone
- Symptoms worsen significantly with weight-bearing activity
- Pain may persist even at rest in advanced cases
- Often accompanied by localized swelling and tenderness
Nerve Compression and Other Causes
Several other conditions can create pain on the top of your foot when walking:
- Nerve entrapment occurs when nerves become compressed by tight footwear or swelling, causing sharp, shooting pain that may extend into your toes.
- Arthritis in the midfoot joints can cause stiffness and pain that worsens with activity, particularly in individuals over 50.
- Ganglion cysts occasionally develop on top of the foot, creating localized pressure and discomfort during walking.
Immediate Pain Relief Strategies
When your foot hurts on top during walking, several immediate strategies can help alleviate pain and reduce inflammation while you determine the underlying cause.
The R.I.C.E. Method
Rest: Temporarily reduce activities that aggravate your symptoms. This doesn’t mean complete bed rest, but avoiding high-impact activities allows inflamed tissues to begin healing.
Ice: Apply ice to the affected area for 15-20 minutes at a time, several times daily during the first 48-72 hours. Always use a barrier between ice and skin to prevent frostbite.
Compression: Gentle compression with an elastic bandage can help reduce swelling. Avoid wrapping too tightly, which can impair circulation.
Elevation: When resting, elevate your foot above heart level to help reduce swelling and improve blood flow.
Footwear Modifications
Improper footwear contributes to 70% of the top of foot pain cases I treat. Making immediate changes to your shoes can provide significant relief:
- Loosen laces: Reduce pressure across the top of your foot by loosening shoe laces or using different lacing techniques.
- Choose supportive shoes: Switch to athletic shoes with good arch support and adequate toe room. Avoid flat shoes or high heels during the acute phase.
- Consider padding: Soft padding over tender areas can reduce direct pressure from shoe contact.
Anti-Inflammatory Measures
Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can help reduce inflammation and manage pain. Follow package directions and consult with healthcare providers if you have medical conditions or take other medications.
Natural anti-inflammatory approaches include:
- Gentle stretching of the foot and calf muscles
- Maintaining good hydration
- Avoiding foods that promote inflammation
Distinguishing Between Conditions: A Diagnostic Guide
Determining whether your pain stems from tendonitis, stress fractures, or other causes is crucial for appropriate treatment. Here’s how we help patients differentiate:
Tendonitis vs. Stress Fracture Assessment
Symptom |
Extensor Tendonitis |
Stress Fracture |
|---|---|---|
| Pain onset | Gradual, activity-related | Progressive, worsening |
| Pain location | Along the tendon pathway | Localized to the bone |
| Rest relief | Significant improvement | Limited improvement |
| Swelling | Mild, along tendons | Localized, over the fracture site |
| Morning stiffness | Common | Less common |
Self-Assessment Questions
Ask yourself these questions to better understand your condition:
- When did the pain start? Sudden onset may indicate acute injury, while gradual development suggests overuse.
- What activities worsen symptoms? Tendonitis typically hurts with toe lifting, while fractures hurt with any weight-bearing.
- Does rest help? Significant improvement with rest suggests tendonitis; persistent pain may indicate a fracture.
- Where exactly does it hurt? Point to the most tender area to help identify affected structures.
When to See a Podiatrist: Red Flag Symptoms
While many cases of top-of-foot pain respond to conservative treatment, certain symptoms require immediate professional evaluation. In my practice, I emphasize that patients should seek urgent care for:
Immediate medical attention needed:
- Inability to bear weight on the affected foot
- Severe pain that doesn’t improve with rest and over-the-counter medication
- Numbness or tingling in the foot or toes
- Signs of infection: warmth, redness, fever, or red streaking
- Deformity or visible bone protrusion
Schedule an appointment within 1-2 days:
- Pain persists longer than 3-5 days despite conservative treatment
- Swelling that doesn’t respond to elevation and ice
- Pain that interferes with sleep or daily activities
- History of diabetes or circulation problems with any foot pain
Professional Treatment Options
When conservative measures aren’t sufficient, several professional treatment options can effectively address pain on top of foot when walking.
Diagnostic Evaluation
My comprehensive evaluation includes:
- Physical examination: Assessment of foot structure, range of motion, and specific areas of tenderness helps identify the exact cause of your symptoms.
- Imaging studies: X-rays rule out fractures and bone abnormalities. MRI or ultrasound may be necessary to visualize soft tissue structures like tendons and ligaments.
- Gait analysis: Observing how you walk helps identify biomechanical factors contributing to your condition.
Non-Surgical Treatments
Physical therapy forms the cornerstone of treatment for many patients. A structured program typically includes:
- Specific stretching exercises for foot and calf muscles
- Strengthening activities to improve foot function
- Biomechanical training to prevent future injuries
- Manual therapy techniques to reduce pain and improve mobility
Custom orthotics address underlying biomechanical problems. According to clinical studies, custom foot orthotics improve symptoms in 85% of patients with chronic foot pain related to structural abnormalities.
Injection therapy may be considered for severe inflammation. Corticosteroid injections can provide significant pain relief, though they require careful consideration due to potential risks to tendon integrity.
Advanced Treatment Options – Top Of Foot Pain
For persistent cases that don’t respond to conservative treatment:
- Immobilization: Walking boots or casts may be necessary for stress fractures or severe tendonitis cases.
- Extracorporeal shock wave therapy: This non-invasive treatment uses sound waves to promote healing in chronic tendonitis cases.
- Surgical intervention: Reserved for cases with structural problems or chronic conditions that haven’t responded to conservative treatment.
Recovery Timeline and Expectations
Understanding what to expect during recovery helps patients stay motivated and recognize normal healing progression.
Week-by-Week Recovery Guide
Week 1-2: Acute Phase
- Focus on rest, ice, and pain management
- Expect a gradual reduction in sharp pain
- Swelling should begin to decrease
- Light, pain-free activities only
Week 3-4: Early Recovery
- Pain should be significantly reduced
- Begin gentle stretching exercises
- Gradually increase walking distance
- May return to low-impact activities
Week 5-8: Progressive Recovery
- Most daily activities should be comfortable
- Can begin strengthening exercises
- Gradual return to sports or high-impact activities
- Focus on prevention strategies
Signs of Healing Progression
Positive indicators that your treatment is working include:
- Decreased pain intensity during rest and activity
- Reduced morning stiffness
- Improved range of motion
- Ability to walk longer distances without discomfort
- Decreased swelling and tenderness
Prevention Strategies for Long-Term Foot Health
With our clinical experience, patients who address prevention factors see 50% faster recovery and significantly lower recurrence rates.
Footwear Selection Guidelines
Proper fit characteristics:
- One thumb-width space between the longest toe and the shoe end
- Adequate width to prevent compression across the top
- Firm heel counter for stability
- Flexible sole that bends at the ball of the foot
Activity-specific recommendations:
- Running shoes: Replace every 300-500 miles
- Work shoes: Choose supportive options for prolonged standing
- Dress shoes: Limit high heel use and ensure proper fit
Activity Progression Principles
- The 10% rule: Increase activity intensity or duration by no more than 10% weekly to allow tissues to adapt gradually.
- Cross-training benefits: Varying activities reduces repetitive stress on specific structures while maintaining fitness.
- Warm-up importance: Five minutes of gentle movement before exercise prepares tissues for increased demands.
Strength and Flexibility Maintenance
Daily foot exercises:
- Toe curls and spreads to maintain flexibility
- Calf stretches against a wall
- Towel scrunches to strengthen small foot muscles
- Alphabet draws with your toes for mobility
Lower leg strengthening: Strong calf and shin muscles support proper foot mechanics and reduce injury risk.
Conclusion: Your Path to Pain-Free Walking
Pain on top of foot when walking is a common but treatable condition that affects people of all activity levels. Understanding the causes, implementing appropriate treatment strategies, and following prevention guidelines can help you return to comfortable, pain-free walking.
Remember that most cases respond well to conservative treatment when properly managed. However, don’t hesitate to seek professional care if your symptoms persist or worsen despite following appropriate self-care measures.
At our podiatry practice, we’re committed to helping patients achieve optimal foot health through comprehensive evaluation, evidence-based treatment, and patient education. If you’re experiencing persistent foot pain that interferes with your activities, contact us to schedule a consultation.
Taking care of your feet is an investment in your overall health and mobility. With the right approach and professional guidance when needed, you can overcome top of foot pain and maintain an active, comfortable lifestyle.
*Medical Disclaimer: This information is for educational purposes only and should not replace professional medical advice. Always consult with a qualified podiatrist or healthcare provider for proper diagnosis and treatment of foot pain conditions.
Frequently Asked Questions About Top Of The Foot Pain
Q. How long does pain on top of foot take to heal?
A. Most cases of extensor tendonitis resolve within 2-4 weeks with appropriate treatment. Stress fractures typically require 6-8 weeks for complete healing. Chronic conditions may take several months, particularly if biomechanical factors aren’t addressed.
Q. Can I continue exercising with top of foot pain?
A: Modify activities to avoid aggravating symptoms. Low-impact exercises like swimming or cycling may be appropriate, while high-impact activities should be avoided until pain resolves.
Q. Will the pain come back?
A: According to research studies, recurrence rates are significantly lower in patients who address underlying causes like improper footwear and biomechanical problems. Following prevention strategies reduces recurrence risk by up to 80%.
Q. Do I need special shoes or orthotics?
A. Many patients benefit from supportive athletic shoes during recovery. Custom orthotics may be recommended if you have structural foot abnormalities like flat feet or high arches that contribute to the problem.
Q. When Home Treatment Isn’t Enough?
A: Despite following conservative treatment measures, some patients require professional intervention. In our practice, we typically recommend a professional evaluation if:
- Symptoms persist longer than two weeks despite appropriate self-care
- Pain interferes with work or daily activities
- You experience recurring episodes of foot pain
- You have underlying conditions like diabetes or circulation problems
Early professional intervention often leads to faster recovery and prevents complications that can develop with prolonged, untreated foot pain.